Can we talk about something that doesn’t get nearly enough attention?
It’s not glamorous. It’s not dinner table conversation. But it affects virtually every man on the planet at some point in his life.
I’m talking about the prostate.
This small, walnut-sized gland sits quietly in your body for decades, doing its job without any fuss. And then, somewhere around midlife, it starts making its presence known. Frequent bathroom trips. Waking up at night. That nagging feeling that something isn’t quite right.
The thing is, prostate issues aren’t inevitable. Or at least, their severity isn’t. There’s so much you can do—starting now, at any age—to support this often-ignored part of your body.
Let’s talk about what the prostate actually does, what can go wrong, and how to keep it healthy for the long haul.
What Is the Prostate, Anyway?
First things first. What exactly is this thing?
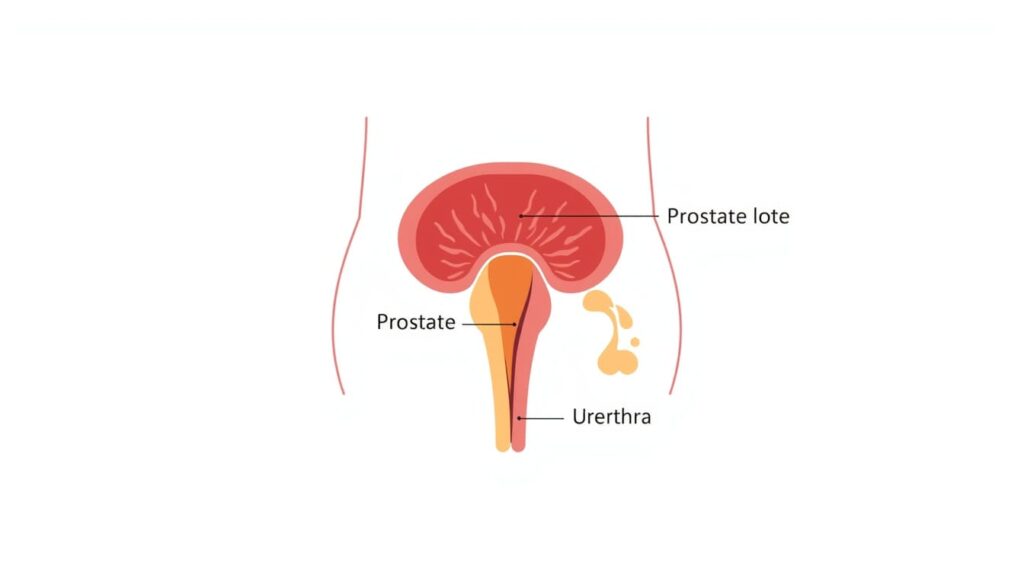
The prostate is a small gland located just below the bladder, surrounding the urethra—the tube that carries urine and semen out of the body. Its main job? To produce fluid that nourishes and transports sperm. That’s it. Small gland, big responsibility.
For most of your life, you don’t think about it at all. It just does its thing. But as you age, the prostate often grows. And because it surrounds the urethra, even slight enlargement can squeeze that tube and cause urinary symptoms.
This is benign prostatic hyperplasia, or BPH—fancy medical speak for an enlarged prostate that isn’t cancer. It’s incredibly common. By age 60, about half of men have some degree of BPH. By age 85, that number jumps to 90 percent.
But here’s the good news: How you live your life can significantly influence how much your prostate enlarges and how bothersome the symptoms become.
The Three Main Prostate Problems
Let’s break down what can go wrong. Knowledge is power.
BPH (Enlarged Prostate). Again, this is non-cancerous growth. Symptoms include frequent urination, especially at night; urgency (feeling like you absolutely have to go right now); weak stream; and feeling like your bladder isn’t completely empty. It’s annoying, but not life-threatening.
Prostatitis. This is inflammation of the prostate, and it can happen at any age—even in young men. It might be caused by bacteria, or it might be chronic pelvic pain with no clear infectious cause. Symptoms include pain in the pelvic area, painful urination, and flu-like symptoms if it’s bacterial.
Prostate Cancer. This is the big one that scares everyone. Prostate cancer is common—it’s the second most common cancer in men worldwide. But here’s what they don’t always tell you: Most prostate cancers grow slowly. Many men die with prostate cancer, not from it. Still, it deserves attention and respect.
The key with all three? Early detection and lifestyle matter immensely.
Diet Matters More Than You Think
If there’s one thing research agrees on, it’s this: What you eat directly affects your prostate.
Tomatoes. They’re rich in lycopene, a powerful antioxidant linked to lower prostate cancer risk. Cooked tomatoes—like in sauce or paste—actually have more available lycopene than raw. Good news for pasta lovers.
Cruciferous vegetables. Broccoli, cauliflower, Brussels sprouts, kale. These contain compounds that help your body detoxify and may protect against cancer. Aim for some every day.
Healthy fats. Fish rich in omega-3s—salmon, sardines, mackerel—reduce inflammation throughout the body, including the prostate. Olive oil, nuts, and avocados also support overall health.
Green tea. Studies suggest that the antioxidants in green tea, especially EGCG, may slow prostate cancer growth. A few cups a week certainly can’t hurt.
Limit dairy and red meat. Some research links high consumption of dairy and red meat to increased prostate cancer risk. You don’t have to eliminate them entirely. Just be mindful of portions and frequency.
Action Step: This week, add one prostate-friendly food to your routine. Maybe it’s a tomato-based sauce. Maybe it’s broccoli with dinner. Maybe it’s swapping one coffee for green tea. Small shifts add up. Our article on The Maqui Berry dives into another antioxidant powerhouse that supports overall health, including inflammation reduction.
The Inflammation Connection
Remember our conversations about inflammation? It shows up everywhere.
Chronic, low-grade inflammation contributes to BPH, prostatitis, and potentially prostate cancer. When your body is inflamed, everything functions less optimally—including that little gland below your bladder.
What drives inflammation? The usual suspects. Processed foods. Sugar. Industrial seed oils. Chronic stress. Poor sleep. Sedentary lifestyle. All of these keep your body in a state of low-level alert, and your prostate pays the price.
The Shift:
Supporting your prostate means supporting your whole body. Anti-inflammatory eating isn’t just about one organ. It’s about creating an internal environment where every system can function well. Check out Thermogenic Resistance: Why Your Metabolism Feels Broken (And How to Fix It) for more on how inflammation affects weight and energy—it’s all connected.
Movement and the Pelvic Floor
Here’s something rarely discussed: Your pelvic floor muscles matter for prostate health.
These muscles support your bladder, bowel, and prostate. When they’re weak or tight, urinary symptoms can worsen. And many men—especially those who sit all day—have pelvic floor issues without realizing it.
Exercise helps in multiple ways.
Cardiovascular exercise. Regular walking, jogging, or cycling improves blood flow to the entire pelvic region. Better blood flow means better nutrient delivery and waste removal.
Pelvic floor exercises. Yes, men can do Kegels too. Learning to contract and relax these muscles can improve urinary control and reduce symptoms of BPH and prostatitis.
Avoid prolonged sitting. Sitting for hours compresses the pelvic area and reduces blood flow. If you have a desk job, stand up and move every hour. Even one minute helps.
Action Step: Add a short walk after meals. It aids digestion, reduces inflammation, and gets blood moving to places that need it. Living Lighter: Practical Tips for Everyday Life has simple ways to weave more movement into your day without overhauling your routine.
Stress and the Prostate
We’ve talked about cortisol many times. Here it is again.
Chronic stress elevates cortisol. Elevated cortisol increases inflammation. Increased inflammation affects every organ, including the prostate. It’s a direct line.
But stress also affects behavior. When you’re stressed, you’re more likely to eat poorly, skip exercise, drink more alcohol, and sleep less—all of which independently harm prostate health.
The Shift:
Managing stress isn’t soft or optional. It’s foundational. Your prostate is literally bathed in the hormonal consequences of your stress levels. Calmer nervous system, calmer prostate. Mental Resilience: Why It’s Essential for Well-Being explores practical ways to build that capacity.
Supplements That Support Prostate Health
Before we talk about specific supplements, a disclaimer: Always talk to your doctor before starting anything new. What works for one person may not work for another.
That said, certain supplements have research behind them for prostate support.
Saw palmetto. This herb is the most studied for BPH. Some research shows it can reduce urinary symptoms, though results are mixed. Many men find it helpful.
Beta-sitosterol. A plant compound that appears to improve urinary flow and symptoms of BPH. Found naturally in many plants, also available as a supplement.
Zinc. The prostate contains higher levels of zinc than any other organ in the body. Adequate zinc is crucial for prostate health. Food sources include oysters, beef, pumpkin seeds.
Vitamin D. Low levels are linked to higher prostate cancer risk. Get your levels checked and supplement if needed.
Action Step: If you’re considering supplements, start with food first. Then talk to a knowledgeable healthcare provider about what might benefit you specifically.
The Importance of Regular Check-Ups
Here’s the uncomfortable truth: You can do everything right and still develop prostate issues. Genetics play a role. Age plays a role. That’s just reality.
But early detection changes outcomes dramatically.
The two main screening tools are the PSA blood test and the digital rectal exam. Neither is perfect. Both have pros and cons. The right age to start screening depends on your risk factors—family history, race, overall health.
The Shift:
Don’t avoid the doctor because you’re nervous. Don’t skip the conversation because it feels awkward. A few minutes of discomfort could save your life. Seriously.
Action Step: If you’re over 40, or younger with family history, schedule a conversation with your doctor about prostate screening. Just a conversation. No commitment. Just information. Mind-Body Integration: The Secret to Living Well talks about listening to your body and honoring its needs—this is part of that.
Putting It All Together
Prostate health isn’t complicated. It’s the same stuff that supports every other part of your body.
Eat real food, mostly plants. Move your body regularly. Manage your stress. Sleep enough. See your doctor. That’s it.
The difference is that men often neglect these basics when it comes to their own health. We’re busy. We’re tough. We don’t want to bother anyone. But your health matters. Your life matters. And the people who love you want you around for a long, long time.
Start where you are. Pick one thing from this article that feels doable. Maybe it’s adding broccoli to dinner. Maybe it’s scheduling that doctor’s appointment you’ve been putting off. Maybe it’s a five-minute walk after lunch. Maybe natural nutrients.
One thing. Just start.
Have you ever talked to your doctor about prostate health? What’s one small step you’re ready to take? Share in the comments—your courage might inspire someone else.


Deja una respuesta